Ankle Problems
Is ankle pain or instability disrupting your life?
Our experienced podiatrists specialize in diagnosing and treating a wide range of ankle problems, including Achilles tendinitis, ankle sprains, and fractures. We offer comprehensive care to help you find relief, recover quickly, and prevent future issues. Discover how our ankle specialists can help you get back on your feet.
Achilles Tendinosis
Achilles tendinosis, also known as Achilles tendonitis, is a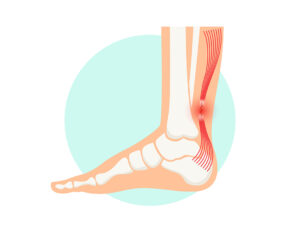 condition characterized by the degeneration and inflammation of the Achilles tendon. The Achilles tendon is a strong band of tissue that connects the calf muscles to the heel bone. Often, a painful spur is present on the back of the heel.
condition characterized by the degeneration and inflammation of the Achilles tendon. The Achilles tendon is a strong band of tissue that connects the calf muscles to the heel bone. Often, a painful spur is present on the back of the heel.
Achilles tendinosis typically occurs due to overuse, repetitive strain, or an acute injury to the tendon. It is a common ankle problem that affects athletes or individuals involved in activities such as jumping, running, or sudden changes in direction.
Symptoms of Achilles tendinosis include pain and stiffness along the back of the heel or lower calf, especially after physical activity or upon waking up in the morning. The area may feel tender to the touch, and swelling or thickening of the tendon may be present.
Treatment for Achilles tendinosis focuses on relieving pain, reducing inflammation, and promoting healing. This may involve resting the affected leg, applying ice to the area, using nonsteroidal anti-inflammatory drugs (NSAIDs) for pain relief, and wearing supportive shoes or orthotic inserts. Physical therapy exercises can also help strengthen the calf muscles and improve flexibility.
In severe or persistent cases, when conservative measures do not provide sufficient relief, medical intervention may be necessary. This can include extracorporeal shockwave therapy, platelet-rich plasma (PRP) injections, or, in rare cases, surgical repair of the tendon.
It is important to seek medical advice if you suspect you have Achilles tendinosis or are experiencing persistent pain and discomfort in the Achilles tendon area. A healthcare professional can provide an accurate diagnosis and recommend appropriate treatment options for your specific condition.
Heel Spur
A heel spur is a bony growth that develops on the underside  of the heel bone. It typically occurs where the plantar fascia, a thick band of tissue that connects the heel bone to the toes, attaches to the heel.
of the heel bone. It typically occurs where the plantar fascia, a thick band of tissue that connects the heel bone to the toes, attaches to the heel.
Heel spurs are often associated with plantar fasciitis, a condition characterized by inflammation of the plantar fascia. The repeated pulling of the plantar fascia on the heel bone can lead to the formation of a bony spur over time.
Heel spurs themselves may not cause pain, but they can contribute to heel pain and discomfort, especially when walking or standing for long periods. The pain is typically felt on the bottom of the heel and may be sharp or dull.
Treatment for heel spurs focuses on managing the underlying condition, such as plantar fasciitis. This may include resting the foot, using orthotic inserts or heel pads for cushioning and support, wearing appropriate footwear, and performing stretching exercises to relieve tension on the plantar fascia. In some cases, physical therapy, anti-inflammatory medications, or corticosteroid injections may be recommended.
It is important to note that not all cases of heel pain are caused by heel spurs. Other factors, such as tight calf muscles, stress fractures, or nerve-related issues, can also contribute to heel pain.
Ankle Joint Pain
Ankle joint pain is extremely common ankle problem. Ankle joint pain is discomfort or soreness felt in the area where your foot connects to your leg. It can range from mild to severe and may be caused by various factors such as injury, inflammation, or medical conditions. The pain can make it difficult to walk, stand, or put weight on the affected ankle.
your foot connects to your leg. It can range from mild to severe and may be caused by various factors such as injury, inflammation, or medical conditions. The pain can make it difficult to walk, stand, or put weight on the affected ankle.
When it comes to treating ankle joint pain, there are a few options available:
1. Rest and self-care: This involves taking a break from activities that worsen the pain, applying ice packs to reduce swelling, and elevating the ankle to relieve pressure.
2. Pain medication: Over-the-counter pain relievers like acetaminophen or non-steroidal anti-inflammatory drugs (NSAIDs) can help reduce pain and inflammation. Always follow the recommended dosage and consult a healthcare professional if needed.
3. Physical therapy: A physical therapist can guide you through exercises and techniques to strengthen the ankle joint, improve flexibility, and promote healing.
4. Supportive devices: Wearing supportive footwear, using ankle braces, or using orthotic inserts can provide stability and reduce stress on the ankle joint during movement.
5. Immobilization: In some cases, a doctor may recommend immobilizing the ankle with a cast, brace, or splint to allow the joint to heal.
6. Injections: Corticosteroid injections may be used to reduce inflammation and provide temporary pain relief. However, they are generally used sparingly due to potential side effects.
7. Surgery: If conservative treatments fail to provide relief, surgery may be considered. Surgical options can vary depending on the specific condition causing the ankle joint pain.
It’s important to note that these are general treatment options, and the most suitable approach will depend on the underlying cause and severity of the ankle joint pain. Consulting with a healthcare professional is crucial for a proper diagnosis and personalized treatment plan.
Fracture
A fracture is a break or crack in a bone. When it affects the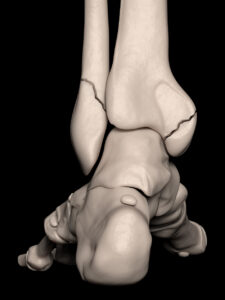 feet, it can cause significant discomfort and affect your ability to walk or stand properly. It may result from accidents, falls, or overuse injuries. Common symptoms of a foot fracture include pain, swelling, bruising, and difficulty bearing weight on the affected foot. Treatment usually involves immobilizing the foot with a cast, brace, or splint to allow the bone to heal. In some cases, surgery may be required. It’s important to seek medical attention for proper diagnosis and treatment of a foot fracture to ensure proper healing and prevent long-term complications. If you think that you may have this ankle problem, consult with a healthcare professional.
feet, it can cause significant discomfort and affect your ability to walk or stand properly. It may result from accidents, falls, or overuse injuries. Common symptoms of a foot fracture include pain, swelling, bruising, and difficulty bearing weight on the affected foot. Treatment usually involves immobilizing the foot with a cast, brace, or splint to allow the bone to heal. In some cases, surgery may be required. It’s important to seek medical attention for proper diagnosis and treatment of a foot fracture to ensure proper healing and prevent long-term complications. If you think that you may have this ankle problem, consult with a healthcare professional.
Sprains/Instability
A sprain or instability in the feet occurs when the ligaments, which are strong bands of tissue that connect bones together, get stretched or torn. This can happen due to sudden twisting or rolling of the foot, causing pain, swelling, and difficulty in walking or putting weight on the affected foot. The foot may feel unstable, and there may be a sensation of the foot giving way.
which are strong bands of tissue that connect bones together, get stretched or torn. This can happen due to sudden twisting or rolling of the foot, causing pain, swelling, and difficulty in walking or putting weight on the affected foot. The foot may feel unstable, and there may be a sensation of the foot giving way.
When it comes to treating ankle sprains and instability, there are a few treatment options:
1. Rest and self-care: Initially, it’s important to rest the ankle and avoid activities that worsen the pain. Applying ice packs, compressing the ankle with a bandage, and elevating the foot can help reduce swelling and discomfort.
2. Pain medication: Over-the-counter pain relievers like acetaminophen or non-steroidal anti-inflammatory drugs (NSAIDs) can help manage pain and reduce inflammation.
3. Physical therapy: A physical therapist can guide you through exercises to improve ankle strength, stability, and range of motion. They may also use techniques like taping or bracing to support the ankle during the healing process.
4. Immobilization: In more severe cases, a doctor may recommend immobilizing the ankle with a brace, splint, or cast to allow the ligaments to heal properly.
5. Rehabilitation exercises: Gradually, as the ankle heals, specific exercises can help improve balance, coordination, and proprioception (awareness of joint position). These exercises can reduce the risk of recurrent sprains and enhance ankle stability.
6. Surgical intervention: In rare cases where conservative measures fail to address ankle instability, surgery may be considered. The surgical procedure can involve repairing or reconstructing damaged ligaments.
It’s important to consult with a healthcare professional for a proper diagnosis and personalized treatment plan, as the severity of the sprain and the extent of ankle instability can vary. Following medical advice and completing the recommended rehabilitation program is crucial for recovery and preventing future ankle problems.
Tendonitis
Tendonitis is one of the most common ankle problems. Tendonitis is the inflammation or irritation of a tendon, which is a thick cord-like structure that connects muscles to bones. It commonly occurs due to overuse or repetitive movements, such as in sports or repetitive job tasks. Tendonitis can cause pain, tenderness, and swelling in the affected area, making it difficult to move the associated joint. Rest, ice, and anti-inflammatory medications are often recommended for initial treatment. Modifying activities, stretching, and physical therapy exercises can help alleviate symptoms and promote healing. In severe cases, a healthcare professional may suggest additional interventions such as corticosteroid injections or, rarely, surgery. It’s important to rest and seek medical advice for proper diagnosis and treatment of tendonitis to prevent further complications.
is a thick cord-like structure that connects muscles to bones. It commonly occurs due to overuse or repetitive movements, such as in sports or repetitive job tasks. Tendonitis can cause pain, tenderness, and swelling in the affected area, making it difficult to move the associated joint. Rest, ice, and anti-inflammatory medications are often recommended for initial treatment. Modifying activities, stretching, and physical therapy exercises can help alleviate symptoms and promote healing. In severe cases, a healthcare professional may suggest additional interventions such as corticosteroid injections or, rarely, surgery. It’s important to rest and seek medical advice for proper diagnosis and treatment of tendonitis to prevent further complications.